
Imagine a world without antibiotics. Before antibiotics, common diseases such as strep throat, an ear infection, or a urinary tract infection could easily lead to death. Alexander Fleming’s fortunate discovery of bacteria-zapping penicillin changed all that in 1928. Today, antibiotics are lifesavers. But now we face a new problem: bacteria are able to adapt to antibiotics. Stronger diseases, super bugs that are resistant to existing antibiotics, threaten us once again.
Many factors contribute to the formation of these drug-resistant bacteria. Some say that doctors are too quick to prescribe antibiotics to treat infections that the body could handle on its own. Others blame patients who use antibiotics improperly, not finishing their entire prescriptions. This improper use allows the strongest bacteria to survive, reproduce, and worst of all, adapt to antibiotics. Bacteria that adapt to antibiotics lead to new strains of drug-resistant diseases like MRSA: the super staph infection.
Back to the Basics: Bacterial Behavior
Bacteria are all around us – on our skin, in our mouths and guts, and throughout our body. We rely on bacteria to help digest our food. We even ingest it in cheese, yogurt, vinegar, and beer. These bacteria are all good. Bad bacteria make us sick by producing chemicals which act like acids.
Bacteria multiply, every few days, hours, or even minutes, making it possible for their population to increase rapidly. Bacteria exchange genetic material between themselves in a process known as transduction (similar to reproduction among mammals). This is how bacteria spread drug resistance amongst one another.
But how does drug resistance happen in the first place? They may be microscopic, but bacteria are complete life forms that undergo chemical processes such as digestion and metabolism. Antibiotics hinder these processes by slowing them down or interrupting them altogether. Different classes of antibiotics target different chemical processes. But bacteria can fight back, targeting each antibiotic’s susceptibility. The bacteria then pass this resistance along to other forms of bacteria. This means trouble for us.
Staph Infections
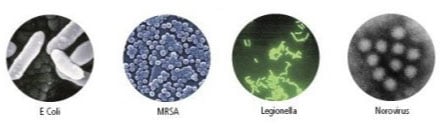
Staphylococcus, typically called “staph,” is a type of bacteria that many healthy individuals commonly carry in their noses or on their skin. Staphylococcus gets its name from its appearance under the microscope: staphyle, the Greek word for a bunch of grapes, combined with kokkos, meaning berry. Twenty-five to 30% of the population is colonized with staph. This means that in roughly a quarter of the population, staph bacteria are present without causing infection.
Illness results when staph bacteria are somehow able to overcome the body’s natural defense mechanisms. Staph-related sicknesses range from skin infections to food poisoning or toxic shock syndrome, and severity ranges from mild to fatal. Over 30 types of staph are able to infect humans, but most are caused by the Staphylococcus aureus variety.
Beginning in the 1940s, penicillin was produced and used to treat Staph aureus. Alarmingly, within just ten years, a drug resistant strain emerged. This strain was also resistant to the newest antibiotics such as erythromycin, streptomycin, and tetracycline. By 1960, methicillin was introduced, but less than twenty years later, Australia reported the first methicillin-resistant strain of staph. Methicillin-resistant Staphylococcus aureus (MRSA) was born, and in a few years it had cropped up all over the world.
Who is at Risk for MRSA?
 Although MRSA has been around for a while, recent fatal outbreaks in schools have brought MRSA into the spotlight once again. Only one effective antibiotic remains: vancomycin. And two cases of staph resistant to this last line of defense have already appeared – in the United States.
Although MRSA has been around for a while, recent fatal outbreaks in schools have brought MRSA into the spotlight once again. Only one effective antibiotic remains: vancomycin. And two cases of staph resistant to this last line of defense have already appeared – in the United States.
Certain groups are definitely more susceptible to staph infections. These include newborns and the elderly, breastfeeding women, and people with chronic conditions such as vascular disease, cancer, lung disease, or diabetes. Individuals with skin disorders, surgical incisions, or an overall weakened immune system also have an increased risk of developing staph infections.
However, otherwise healthy individuals are also able to contract staph infections. Although it’s usually treatable, when MRSA enters the bloodstream, the infection is life-threatening. This is why it is important to be aware of how staph infections develop and how to prevent them. Once someone contracts a staph infection, anyone in close contact with them can contract it from them. Athletes and prisoners fall into this category of high-risk for contraction, and so do family members and coworkers.
In fact, there is a special designation for MRSA contracted by those who have not been in a healthcare-related environment – community-associated MRSA (CA-MRSA). The Centers for Disease Control (CDC) estimates that around 12% of MRSA cases now fall within this category. But the vast majority of MRSA cases appear in healthcare settings.
The Transmission of MRSA
 The National Institute for Occupational Safety and Health (NIOSH) reports “5 Cs” that make it easier for the disease to be transmitted: Crowding, frequent skin-to-skin Contact, Compromised skin, Contaminated items and surfaces, and lack of Cleanliness.
The National Institute for Occupational Safety and Health (NIOSH) reports “5 Cs” that make it easier for the disease to be transmitted: Crowding, frequent skin-to-skin Contact, Compromised skin, Contaminated items and surfaces, and lack of Cleanliness.
When there is a cut or abrasion on the skin, staph bacteria can make their way into the wound. If the infection reaches the bloodstream, the condition is very serious. As one spokeswoman for the Tulsa City-County Health Department put it: “For the majority of healthy people, MRSA is treatable. There is always a concern because it can become invasive, which can be fatal.”
Symptoms and Treatment of MRSA
MRSA infections appear on the surface of the skin as pustules or boils that are usually red and swollen. Staph infections are painful from the start, making them easy to detect. Staph infections may or may not be treated with antibiotics. Sometimes drainage of boils or abscesses is sufficient treatment (this should only be done by a healthcare provider).
Prevention of MRSA
 The most important, all-encompassing matter in preventing staph infections like MRSA is cleanliness.
The most important, all-encompassing matter in preventing staph infections like MRSA is cleanliness.
Donna Rheaume, spokeswoman for the Department of Public Health, sums it up this way: “The key is prevention, practicing some basic hygiene, and good wound care. I can tell you, we have seen an increase in both hospital- and community-acquired MRSA, so we’re stressing prevention.”
Basic good personal hygiene is the key to preventing MRSA infections. The NIOSH recommends:
- Keep your hands clean by washing them thoroughly with soap and water or by using an alcohol-based sanitizer.
- Keep cuts and scrapes clean and covered with a bandage until they are fully healed.
- Avoid contact with other people’s wounds or bandages.
- Avoid sharing personal items such as uniforms, razors, towels, and the like.
- Wash uniforms and sports equipment frequently.
However, because not all people take these precautions, it is also crucial to maintain a clean environment. The CDC states that it’s critical to maintain a clean environment “by establishing cleaning procedures for frequently touched surfaces and surfaces that come into direct contact with people’s skin.”
The CDC also stresses that “cleaning contaminated equipment and surfaces with detergent-based cleaners or Environmental Protection Agency (EPA)-registered disinfectants is effective at removing MRSA from the environment.” Since MRSA can stay on environmental surfaces for weeks, it is recommended that environmental surfaces that come in direct contact with the skin should be cleaned and disinfected frequently.
However, some disinfectants can be harmful in themselves, often causing skin irritation and even inducing asthma attacks. Vital Oxide is a safe, effective, EPA-approved, broad-spectrum cleaner that kills staph bacteria without any harmful byproducts.
